Review What safety assessments should be completed on the patient prior to assisting with ambulation to the restroom?
Kinh Nghiệm về What safety assessments should be completed on the patient prior to assisting with ambulation to the restroom? Chi Tiết
Bùi Mạnh Hùng đang tìm kiếm từ khóa What safety assessments should be completed on the patient prior to assisting with ambulation to the restroom? được Update vào lúc : 2022-09-26 13:44:05 . Với phương châm chia sẻ Bí quyết về trong nội dung bài viết một cách Chi Tiết 2022. Nếu sau khi đọc tài liệu vẫn ko hiểu thì hoàn toàn có thể lại Comment ở cuối bài để Ad lý giải và hướng dẫn lại nha. Some patients have incontinence, or urgency of bowel or bladder, causing them to hurry to the bathroom. For some, this problem can be compounded by mobility impairments that make ambulating to the bathroom or transferring on/off a toilet or commode
challenging. These impairments may be long-standing for the patient, or acute changes due to the patient’s medical condition. Medication side effects could even be contributing to the problem. A list of interventions that may be of benefit to these patients include: Nội dung chính
Some patients have incontinence, or urgency of bowel or bladder, causing them to hurry to the bathroom. For some, this problem can be compounded by mobility impairments that make ambulating to the bathroom or transferring on/off a toilet or commode
challenging. These impairments may be long-standing for the patient, or acute changes due to the patient’s medical condition. Medication side effects could even be contributing to the problem. A list of interventions that may be of benefit to these patients include: Nội dung chính - Fall Prevention StrategiesTable 3.7 Fall Prevention StrategiesLowering a Patient to the FloorChecklist 31: Lowering a Patient to the FloorCritical Thinking ExercisesWhat should you check prior to ambulating a patient?What steps will you perform to ensure safety during ambulation?What should I do before ambulation?
Patient falls are the most reported patient safety events in British Columbia and account for 40% of all adverse events (BCPSLS, 2015). Falls are a major priority in health care, and health care providers are responsible for identifying, managing, and eliminating potential hazards to patients. All patient-handling activities (positioning, transfers, and ambulation) pose a risk to patients and health care providers. Older adults may be increased risk for falls due to impaired mental status, decreased strength, impaired balance and mobility, and decreased sensory perception (Titler, Shever, Kanak, Picone, & Qin, 2011). Other patients may be risk due to gait problems, cognitive ability, visual problems, urinary frequency, generalized weakness, and cognitive dysfunction. Specific treatments and medications may cause hypotension or drowsiness, which increase a patient’s risk for falls (Hook & Winchel, 2006).
Fall Prevention Strategies
All clients should be assessed for risk factors, and necessary prevention measures should be implemented as per agency policy. Table 3.7 lists factors that affect patient safety and general measures to prevent falls in health care.
Table 3.7 Fall Prevention Strategies
Prior to ambulation consider the following risk factors:- Age (elderly)Sensory-perception alterationCognitive impairment (decreased LOC, confusion)Poly-pharmacologyUrinary incontinenceAbility to communicate (language barriers)Lack of safety awareness (height of bed, attachments and tubes)Environmental factors (dim light, tripping hazards, uneven floors)
 Proper Footwear
Communicate with your patients.
Let patients know when you will be back, and how you will help them ambulate
Keep bed in the lowest position for sedated, unconscious, or compromised patients.
This step prevents injury to patients.
Avoid using side rails when a patient is confused.
Side rails may create a barrier that can be easily climbed and create a fall risk situation for confused patients.
Keep assistive devices and other commonly used items close by.
Allow patients to access assistive devices quickly and safely. Items such as the call bell, water, and Kleenex should be kept close by, to avoid any excessive reaching.
Data source: Accreditation Canada, 2014; Canadian Patient Safety Institute, 2015; Perry et al., 2014; Titler et al., 2011
Proper Footwear
Communicate with your patients.
Let patients know when you will be back, and how you will help them ambulate
Keep bed in the lowest position for sedated, unconscious, or compromised patients.
This step prevents injury to patients.
Avoid using side rails when a patient is confused.
Side rails may create a barrier that can be easily climbed and create a fall risk situation for confused patients.
Keep assistive devices and other commonly used items close by.
Allow patients to access assistive devices quickly and safely. Items such as the call bell, water, and Kleenex should be kept close by, to avoid any excessive reaching.
Data source: Accreditation Canada, 2014; Canadian Patient Safety Institute, 2015; Perry et al., 2014; Titler et al., 2011
Lowering a Patient to the Floor
A patient may fall while ambulating or being transferred from one surface to another. If a patient begins to fall from a standing position, do not attempt to stop the fall or catch the patient. Instead, control the fall by lowering the patient to the floor. Checklist 31 lists the steps to assisting a patient to the floor to minimize injury to patient and health care provider (PHSA, 2010).
Checklist 31: Lowering a Patient to the Floor
Disclaimer: Always review and follow your hospital policy regarding this specific skill.
Safety considerations:- There is always a potential fall risk during transfers and ambulation. Prevention is key.If a patient begins to feel dizzy, have them sit on a chair or the floor to avoid a fall.The head is the most important part of the body toàn thân; always protect it as much as possible.In the sự kiện of a fall, stay with the patient until help arrives.After a fall, always assess a patient for
injuries prior to moving them. If the patient remains weak or dizzy, do not attempt to ambulate them. Seek help.
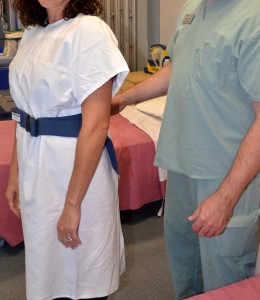 Stand behind
patient
2. Support the patient around the waist or hip area, or grab the gait belt. Bend your leg and place it in between the patient’s legs.
Hand placement allows for a solid grip on the patient to guide the fall.
Stand behind
patient
2. Support the patient around the waist or hip area, or grab the gait belt. Bend your leg and place it in between the patient’s legs.
Hand placement allows for a solid grip on the patient to guide the fall. 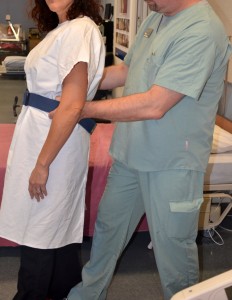 Support patient by grabbing the hip area or gait belt
3. Slowly slide the patient down your leg, lowering yourself the same time. Always protect the head first.
Lowering yourself with the patient prevents back injury and allows you to protect the patient’s head from hitting the floor or hard objects.
Support patient by grabbing the hip area or gait belt
3. Slowly slide the patient down your leg, lowering yourself the same time. Always protect the head first.
Lowering yourself with the patient prevents back injury and allows you to protect the patient’s head from hitting the floor or hard objects. 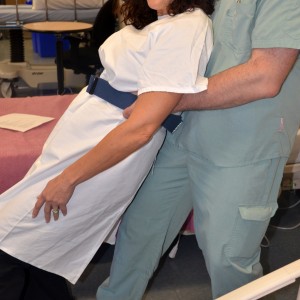 Lower patient to the floor
4. Once the patient is on the floor, assess the patient for injuries prior to moving.
Assesses patient’s ability, or need for additional help, to get off the floor.
Lower patient to the floor
4. Once the patient is on the floor, assess the patient for injuries prior to moving.
Assesses patient’s ability, or need for additional help, to get off the floor.  Assess patient prior to moving
5. Provide reassurance and seek assistance if required.
If required, stay with the patient and call out for help.
6. If patient is unable to get up off the floor, use a mechanical lift.
If patient still feels dizzy or weak, using a mechanical lift will prevent injury.
7. Complete an incident report according to agency policy.
An incident report helps identify and manage risks related to patient falls.
Data source: Perry et al., 2014; PHSA, 2010; Titler et al., 2011
Special considerations:
Assess patient prior to moving
5. Provide reassurance and seek assistance if required.
If required, stay with the patient and call out for help.
6. If patient is unable to get up off the floor, use a mechanical lift.
If patient still feels dizzy or weak, using a mechanical lift will prevent injury.
7. Complete an incident report according to agency policy.
An incident report helps identify and manage risks related to patient falls.
Data source: Perry et al., 2014; PHSA, 2010; Titler et al., 2011
Special considerations:- Use a falls risk assessment tool for all patients according to agency policy.Younger patients may not be aware of the effects of medication and treatments leading to dizziness and orthostatic hypotension.Inform patients and family members about the potential risks for falls in the hospital. If informed, people are more likely to call for assistance.Always ensure call bell is in place. Many falls occur
due to incontinence issues. The call bell allows patient and family to obtain assistance quickly.If appropriate, educate patient about home maintenance and safety to prevent falls when returning home.Fall prevention is interdisciplinary. Proper communication by the care team is required to prevent falls.
Take this Lowering a Patient to the Floor course for more information on lowering a falling patient to the floor.
Critical Thinking Exercises
Name four fall prevention strategies that will help keep a patient safe when ambulating in the hospital.A patient is ambulating for the first time after surgery. Is it safe to encourage the patient to ambulate independently?Many physiological risk factors can be identified from a routine assessment. Name three risk factors and three prevention strategies to manage these risks. For example, if a patient has frequent toileting needs, a preventive action is to offer assistance to the toilet every hour, and to ensure the call bell is within reach all times.What should you check prior to ambulating a patient?
Prior to assisting a patient to ambulate, it is important to perform a patient risk assessment to determine how much assistance will be required. An assessment can evaluate a patient's muscle strength, activity tolerance, and ability to move, as well as the need to use assistive devices or find additional help.What steps will you perform to ensure safety during ambulation?
Safety. Obtain and become familiar with the gait belt to be used.. Assess the patient to make sure he or she is rested and not fatigued.. Obtain extra personnel to assist with ambulation if necessary.. Place bed in the low position with the bed wheels locked.. Address the patient's fear of falling if present..What should I do before ambulation?
Before ambulating ask the patient if they feel dizzy or lightheaded. If they do, sit patient back down on the bed. If patient feels stable, begin walking, matching your steps to the patient's. Tải thêm tài liệu liên quan đến nội dung bài viết What safety assessments should be completed on the patient prior to assisting with ambulation to the restroom? Purpose of ambulation Safe ambulation techniques Ambulation Nursing interventions Ambulate patient meaning Ambulation
Post a Comment